Introduction
Imagine an annual visit to your healthcare provider where one exam could catch early warning signs of cervical cancer, while another offers a comprehensive snapshot of your reproductive health. That’s why understanding the nuances of Pap Smear vs. Pelvic Exam: What’s the Difference and Why Both Matter matters so much—not just to clinicians, but to everyone with a cervix. Clearing up the distinction empowers individuals to advocate for precise, meaningful care, rather than conflating two vital—but different—procedures.
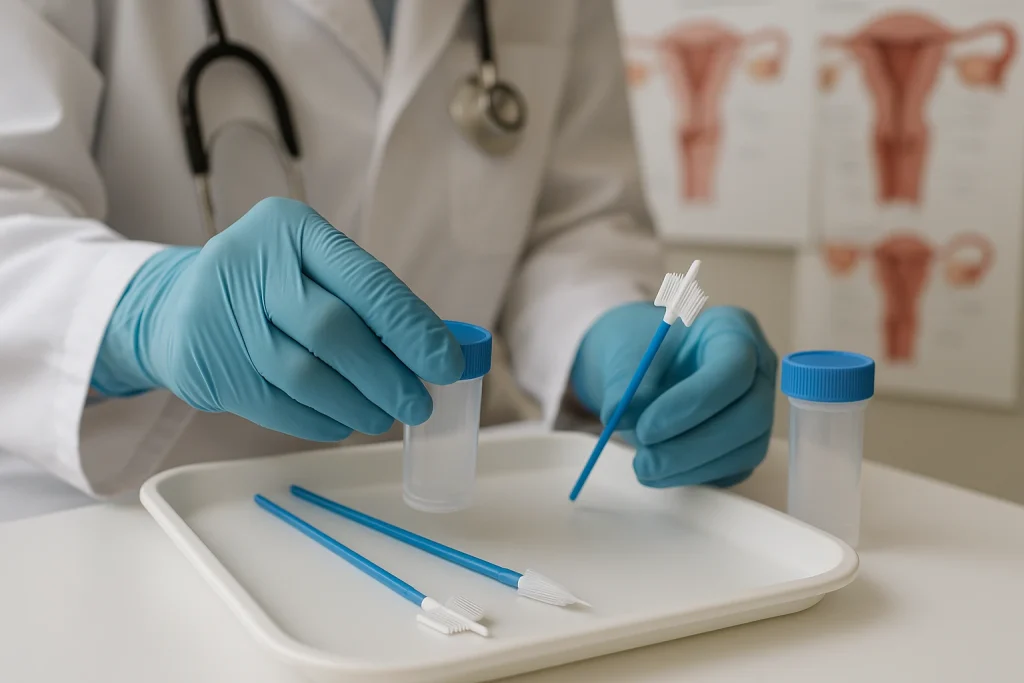
In practice, a Pap smear is a[cell-focused screening tool designed to detect precancerous or cancerous changes in the cervix
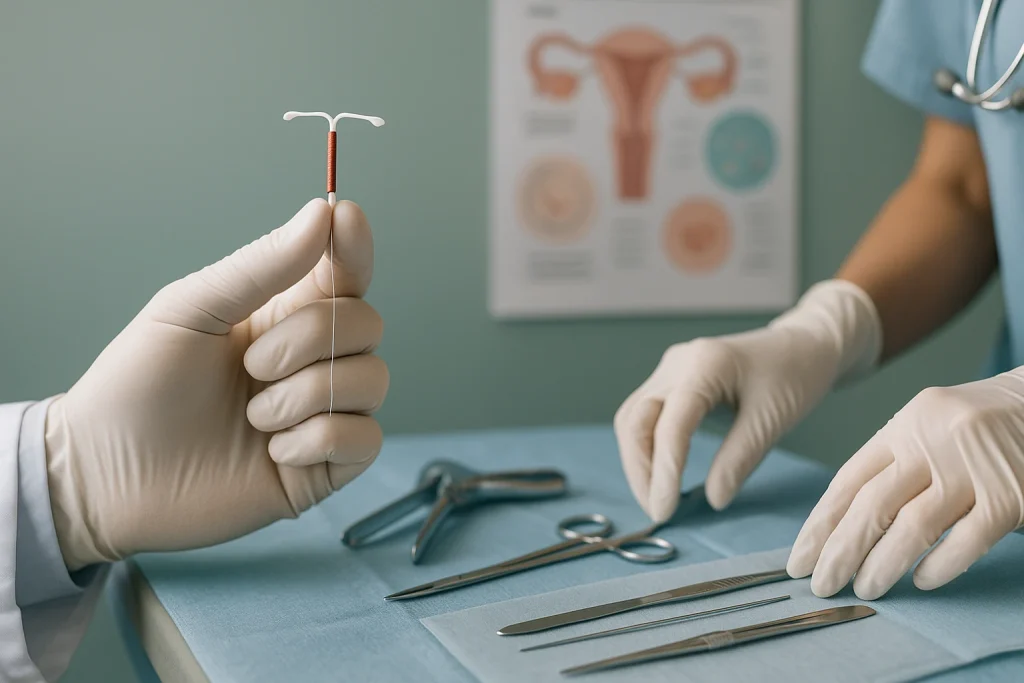
—a lifesaving measure for early detection. According to the Mayo Clinic, a Pap smear collects cervical cells to identify abnormal changes before they progress to cancer (Mayo Clinic). Now compare that to a pelvic exam, which is broader in scope: a physical evaluation of the vulva, vagina, cervix, uterus, and ovaries that goes beyond screening alone. As described by the Cleveland Clinic, a pelvic exam assesses structural and symptomatic concerns, such as ovarian cysts, uterine fibroids, or infections—some of which a Pap smear cannot detect (Cleveland Clinic).
Understanding the interplay between these two exams is critical. For example, a woman in her early 20s may receive her first Pap smear during a well-woman visit, which typically includes a pelvic exam to assess menstrual pain or irregular bleeding. In contrast, someone experiencing pelvic pain but with a recent normal Pap smear may undergo a pelvic exam to explore conditions like ovarian cysts or pelvic inflammatory disease. The mutual reinforcement of screening and diagnostic insights ensures that care is both preventive and responsive.
By exploring Pap Smear vs. Pelvic Exam: What’s the Difference and Why Both Matter, this article will guide readers through how each procedure contributes uniquely to reproductive health—highlighting why they’re not interchangeable, but rather complementary components of comprehensive care. With real clinical examples, evidence-based recommendations, and patient-focused context ahead, it’s time to move beyond confusion to clarity.
Why Both Matter: Clinical Impact of Pap Smear and Pelvic Exam
Understanding the distinction between these two procedures reveals how they complement each other in advancing reproductive healthcare. While the pelvic exam offers a broad physical assessment of the reproductive organs, the Pap smear adds microscopic precision. For instance, a pelvic exam—conducted via visual inspection, speculum insertion, and bimanual palpation—can detect structural concerns such as ovarian cysts, uterine fibroids, or adnexal masses en.wikipedia.org. Meanwhile, the Pap smear targets cellular abnormalities on the cervix, enabling early detection of precancerous changes and cervical cancer—thereby significantly reducing mortality when combined with regular screening and follow-up en.wikipedia.org.
In real-world clinical settings, these exams frequently occur together, though their purposes differ. Take a well-woman visit: the provider may perform a Pap smear as part of cervical cancer screening and then conduct a pelvic exam to evaluate symptoms such as pelvic pain, abnormal bleeding, or discharge my.clevelandclinic.org. For example, a 35-year-old patient reporting irregular bleeding may benefit from the Pap smear identifying potential cytological changes, while the pelvic exam reveals fibroids or endometrial irregularities. This dual approach ensures both microscopic and macroscopic assessment—minimizing missed diagnoses.
| Procedure | Main Purpose | Examples of Findings | Recommended Frequency |
|---|---|---|---|
| Pap Smear | Detects cellular abnormalities on cervix | Precancerous cells, cervical cancer | Every 3 years (ages 21–29); every 3–5 years (ages 30–65) depending on HPV co-testing en.wikipedia.org |
| Pelvic Exam | Physical evaluation of reproductive organs | Fibroids, infections, cysts, pelvic masses | Based on symptoms or annually as part of well-woman care my.clevelandclinic.org |
In light of the common misunderstanding around these procedures, many patients—especially younger individuals—perceive the Pap smear and pelvic exam as synonymous. A 2002 study revealed that only 2.7% of surveyed adolescent girls could accurately define a Pap smear, with 68% believing it was identical to a pelvic exam jamanetwork.com. Clarifying this distinction is essential to ensure informed participation in preventive care.
Moreover, guidelines caution against unnecessary testing. Conducting Pap smears or bimanual pelvic exams in asymptomatic adolescents or women under 21 can lead to anxiety, false positives, and unwarranted treatments cdc.gov. Shared decision-making between providers and patients becomes crucial to applying these procedures appropriately—balancing benefits and potential harms.
In sum, while some might conflate Pap smear vs. pelvic exam: what’s the difference and why both matter, the value of each lies in what it reveals—together providing a fuller, more effective snapshot of reproductive health. Their combined use enhances early detection and patient-centered care through both microscopic insights and physical evaluation.
Understanding the Differences
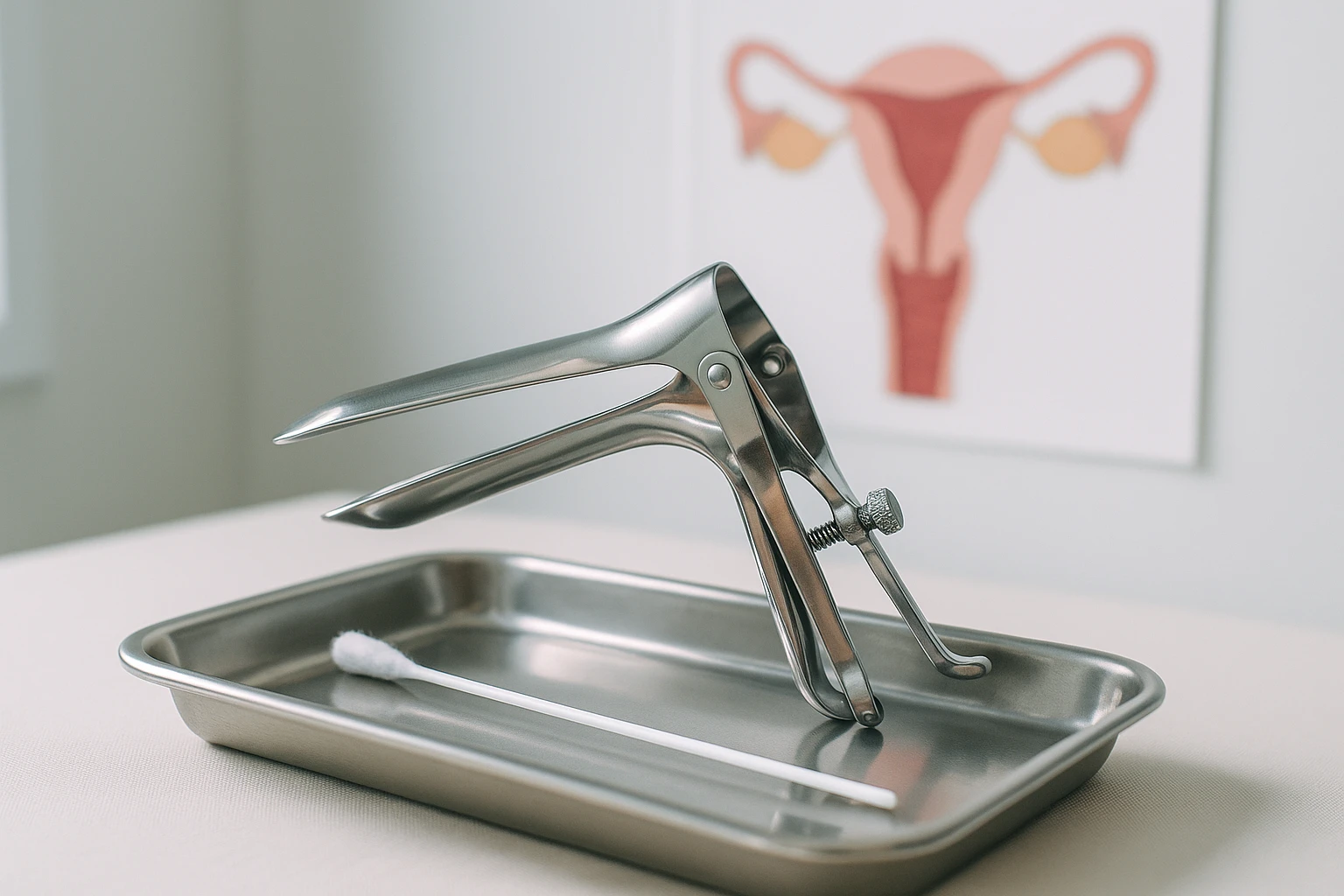
When comparing a Pap Smear vs. Pelvic Exam: What’s the Difference and Why Both Matter, it’s crucial to understand the specific purposes and components of each procedure. A Pap smear is primarily designed to detect cervical cancer by collecting cells from the cervix and examining them for pre-cancerous or cancerous changes. This simple yet effective test is typically recommended for women starting at age 21, with a frequency that depends on age and prior test results. Regular Pap smears have significantly contributed to the decline of cervical cancer rates, as they allow for early intervention and treatment.
In contrast, a pelvic exam has a broader scope and is conducted to assess the health of the female reproductive organs. During this exam, a healthcare provider examines the vulva, vagina, cervix, uterus, and ovaries by using a speculum for better visibility and often including a manual examination. This comprehensive check aims to identify abnormalities such as cysts, sexually transmitted infections, or other potential health issues. Pelvic exams are generally part of a routine gynecological examination and may occur more frequently depending on individual health needs.
The Importance of Both Procedures
The distinction between these two procedures emphasizes the value they provide in maintaining women’s health. While the Pap smear is specifically targeted at cervical cancer prevention, the pelvic exam offers a broader assessment of reproductive health. According to the American Cancer Society, consistent screening and exams have led to a substantial drop in cervical cancer mortality rates, showcasing both the individual and community-level benefits of these health practices.
Many healthcare providers, like those at MedHaven, facilitate comprehensive women’s health care by integrating these essential services into regular health check-ups. This holistic approach ensures that women receive thorough evaluations, allowing for timely discoveries of potential health issues beyond cervical cancer.
Real-World Implications
Real-world cases exemplify the critical role of these exams. For instance, a patient may receive a normal Pap test result but still have an ovarian cyst detected during a pelvic exam, underscoring the significance of both procedures working in concert. As reported by the Harvard Health Blog, skipping regular exams often delays the identification of manageable issues, which can complicate treatment.
By undergoing both Pap smears and pelvic exams, women empower themselves with preventive measures that enhance their long-term health. Understanding these differences allows them to make more informed decisions about their healthcare, ensuring they remain proactive in their wellness journey.
Clinical Implications and Decision-Making: Practical Insights
Building on the understanding of Pap smears and pelvic exams, this section provides actionable insights and real-world decision-making strategies that guide women in collaboration with their healthcare providers. Employing the phrase naturally, we see how informed choices around Pap Smear vs. Pelvic Exam: What’s the Difference and Why Both Matter enable personalized care.
Tailoring Screening Based on Age and Risk
Clinicians typically recommend starting Pap smears at age 21 and repeating them every three years if results remain normal. From age 30 onward, combining Pap tests with HPV testing allows spacing to every five years when both are negative, up to around age 65 health.clevelandclinic.org. In contrast, routine pelvic exams are no longer universally required. For example, asymptomatic women engaged in routine Pap screening may postpone pelvic exams unless specific concerns arise community.the-hospitalist.org.
Recognizing When Pelvic Exams Are Essential
There are clear scenarios in which a pelvic exam provides distinct diagnostic value. Symptoms such as unexplained pelvic pain, abnormal bleeding, discomfort during intercourse, or issues with bladder function necessitate a thorough evaluation including bimanual palpation and external inspection health.clevelandclinic.org. These exams can detect conditions—such as ovarian cysts, uterine fibroids, endometriosis, or vulvar abnormalities—that a Pap smear cannot identify aafp.org.
Avoiding Harm from Over-Screening in Young Women
Evidence points to excessive Pap tests and pelvic exams among young, asymptomatic women, especially those under age 21, resulting in unnecessary costs and potential psychological distress. A study found that around 72% of Pap tests and 54% of pelvic exams in this group may have lacked medical indication aafp.org. These findings underscore the importance of aligning screening frequency with established guidelines and avoiding overuse.
Effective Shared Decision-Making in Practice
Healthcare professionals and patients can benefit from discussing the relative value and discomfort of pelvic exams candidly. Many women appreciate that pelvic exams are optional in the absence of symptoms, yet also value them as opportunities to raise concerns about sexual health, contraception, or pelvic wellness washingtonpost.com. Clinicians should respect patient preferences while weighing clinical indications and maintaining preventive care continuity.
Summary: Aligning Practice with Personalized Care
Understanding Pap Smear vs. Pelvic Exam: What’s the Difference and Why Both Matter equips women to pursue healthcare aligned with guidelines, symptomatology, and personal comfort. The Pap smear remains the gold standard for cervical cancer prevention, while pelvic exams hold targeted diagnostic relevance. Through risk-based scheduling, symptom awareness, and shared decision-making, women and providers can navigate both screenings wisely and efficiently.

Conclusion: The Vital Role of Regular Screenings
Understanding the distinction between a Pap smear and a pelvic exam is crucial for proactive healthcare management. While both play critical roles in diagnosing and preventing various health issues, each has a unique purpose. A Pap smear specifically screens for cervical cancer by detecting abnormal cells, whereas a pelvic exam provides a broader assessment of reproductive and sexual health.
Key Takeaways for Women’s Health
Regular screenings in the form of both Pap smears and pelvic exams are integral to maintaining good health. For example, a Pap smear can detect potentially pre-cancerous changes early, allowing for intervention before cancer develops, thus saving lives. On the other hand, a pelvic exam can uncover other conditions such as infections, cysts, or fibroids, ensuring a comprehensive health overview. As women age, these exams can become even more important in managing changes in health status.
Actionable Insights
It is recommended to schedule these exams according to guidelines provided by healthcare professionals, typically every three years for a Pap smear for women aged 21 to 65. However, individual health history may dictate a different schedule. Stay informed about updates in screening guidelines and discuss any changes with your healthcare provider. Creating an annual or bi-annual health checkup plan can help in tracking this important aspect of health care.
Taking the Next Step
For those looking to be proactive about their health, consider leveraging resources like MedHaven to understand more about Pap smears and pelvic exams. MedHaven offers comprehensive support and resources for making informed decisions, setting up appointments, and accessing expert healthcare advice. This step is essential to ensure you are making the most out of these critical health examinations.
Ultimately, prioritizing both Pap smears and pelvic exams is key to comprehensive healthcare. By staying informed, adhering to recommended screening schedules, and utilizing supportive resources, you can significantly enhance your overall health and well-being.

CRNP, FNP-BC, MSN is a board-certified Family Nurse Practitioner with 16+ years of experience. She provides personalized, high-quality care in family medicine, preventive health, and chronic disease management at MedHaven Health in Glen Burnie, Maryland. Read More